In Conventional Oncology, Bladder cancer is staged (classified by the extent of spread of the cancer) and graded (how abnormal and aggressive the cells appear under the microscope). In this perspective, “Staging” describes where the cancer is located and whether or not it has spread to parts of the body such as the lymph nodes. The conventional purpose of cancer staging is to help determine what kind of treatment should be most effective. Most doctors determine a patient’s cancer stage using the TNM system (which stands for tumor, node, metastasis), which describes the presence of primary tumors, their location, and if they have metastasized. There are four bladder cancer stages that someone can be diagnosed with:
Stage 0a or 0b: This is an early stage when the cancer is on the inner lining of the bladder but has not invaded the muscle or connective tissue.
Stage I: The cancer has grown through the inner lining of the bladder into the lamina propria (a loose layer of connective tissue under the basement membrane lining of the epithelium).
Stage II: The cancer has spread into the thick muscle wall of the bladder, but not the lymph nodes or other organs.
Stage III: The cancer has spread throughout the muscle wall to the fatty layer of tissue surrounding the bladder.
Stage IV: The tumor has spread to the pelvic wall or the abdominal wall, possibly to one or more regional lymph nodes, and potentially to other parts of the body. (Source)
In the TNM staging system for bladder cancer, the following apply
Source for this section fome from this reference (Longe, Jacqueline L. (2005). Gale Encyclopedia Of Cancer: A Guide To Cancer And Its Treatments. Detroit: Thomson Gale. p. 137. (Source).
T (Primary tumour)
TX Primary tumour cannot be assessed
T0 No evidence of primary tumour
Ta Non-invasive papillary carcinoma
Tis Carcinoma in situ (‘flat tumour’)
T1 Tumour invades subepithelial connective tissue
T2a Tumour invades superficial muscle (inner half)
T2b Tumour invades deep muscle (outer half)
T3 Tumour invades perivesical tissue:
T3a Microscopically
T3b Macroscopically (extravesical mass)
T4a Tumour invades prostate, uterus or vagina
T4b Tumour invades pelvic wall or abdominal wall
N (Lymph nodes)
NX Regional lymph nodes cannot be assessed
N0 No regional lymph node metastasis
N1 Metastasis in a single lymph node 2 cm or less in greatest dimension
N2 Metastasis in a single lymph node more than 2 cm but not more than 5 cm in greatest dimension, or multiple lymph nodes, none more than 5 cm in greatest dimension
N3 Metastasis in a lymph node more than 5 cm in greatest dimension
M (Distant metastasis)
MX Distant metastasis cannot be assessed
M0 No distant metastasis
M1 Distant metastasis.
Numerical
The stages above can be integrated into a numerical staging (with Roman numerals) as follows
Stage 0a: Ta, N0, M0
Stage 0is: Tis, N0, M0
Stage I: T1, N0, M0
Stage II: T2a or T2b, N0, M0
Stage III: T3a, T3b, or T4a, N0, M0
Stage IV; any of the following:
T4b, N0, M0
any T, N1 to N3, M0
any T, any N, M1
(Source:“How is bladder cancer staged?”. American Cancer Society. Archived from the original on 4 October 2015. Last Medical Review: 02/26/2014)

Stage N1 bladder cancer

Advanced bladder cancer
Bladder cancer can also be described using grades:
Papilloma — May recur but has a low risk of progressing.
Low grade — Less likely to recur and progress.
High grade — Most likely to recur and progress.
WHO Classification
By the WHO classification of 1973, bladder cancers are histologically graded into the following
G1 – Well differentiated,
G2 – Moderately differentiated
G3 – Poorly differentiated
(Source: Seth P. Lerner. “Overview of Diagnosis and Management of Non-Muscle Invasive Bladder Cancer” (PDF). Food and Drug Administration. ODAC September 14, 2016)
As of 2010 there is insufficient evidence to determine if screening for bladder cancer in people without symptoms is effective or not. (Chou R, Dana T (October 2010). “Screening adults for bladder cancer: a review of the evidence for the U.S. preventive services task force”. Ann. Intern. Med. 153 (7): 461–8. (Source)
In 2013 a preliminary, small study of 98 samples of urine, all from men—24 who had cancer, and 74 with bladder-related problems but no cancer yet used a gas chromatograph to successfully examine the vapor from heated urine samples to identify cancer. (Roberts, Michelle; online (9 July 2013). “Urine odour test for bladder cancer”. BBC News..
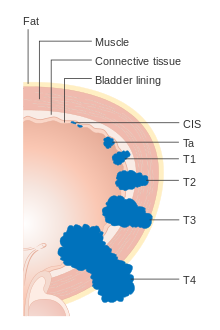
Diagram showing the T stages of bladder cancer
Discussion and Conclusion
As we saw, staging of bladder cancer is typically determined by medical imaging such as CT scan and bone scan. But because CT scans carry a lot of radiation, (See CT test file) and tissue biopsies spread cancer cells, finding non invasive methods to diagnose this type of cancer would therefore be helpful, and all the more that contrast material, especially for MRIs are not healthy. furthermore, PEP scans necessitate an abundance of toxic dye-empregnated glucose sugary solution that feeds the cancer, so the ACR Institute in general also prefers staying away from CT scans and excisional biopsies unless clinically necessary, when the patient’s life is in measurable danger in terms of vital signs.
The approach the ACR Institute prefers is a non invasive one that does not spur cancer growth, whether it be biopsies or radiation devices. Conventional oncologists claim that there are no non invasive tools to diagnose this cancer. So how can we not harm the body, not spread the cancer, and at the same time treat the cancer ?
Because there are a few clinical signs of bladder cancer, the Institute’s approach would be to intensify the HIP protocol when these symptoms emerge while preventing bladder cancer from ever appearing with a simple holistic lifestyle. Epidemiology evidence has shown that toxemia is generally the trigger cause of this cancer. (Source). Therefore, by minimizing toxemia, drinking lots of clean water and having a holistic lifestyle, the risks of contracting this cancer is very low. And then, when there are signs like urine bleeding, back pain, an over-acting bladder and incontenance, the precautionary principle would command that the patient assumes something is wrong, like bladder cancer and promptly start the control and reversal HIP protocol. Using “liquid biopsies” (blood draws to verify the level of circulatory tumor cells) would also be a prudent accompaniment.
We have observed over the decades that too many cancer patients and their doctors, including functional physicians, are obsessed with testing. And then when the result is bad, the patient is so traumatized that it makes any holistic protocol more difficult to prosper. So at the ACR Institute, we prefer to stay away from bad news.
To be vigilant yes, to monitor progress from a baseline, yes, to order medical imagery when there’s a credible evidence-based threat or complication, yes, but to bombard the weakened patient with invasive diagnostic -procedures and then finish off with a double whammy on a bad traumatizing “verdict” that necessitates an onslaught of life-strengthening and tissue damaging procedures (chemo poison, cancer-radiation and traumatizing surgery) is not the holistic way to go, at least this is the ACR Institute’s first-amendment protected informed opinion.
Given the cash-flow model for mainstream medicine as well as liability issues, conventional treatment experts insist on performing a plethora of invasive tests thanks to which they can then stage and grade the cancer, thanks to which they can then start an aggressive and even more invasive treatment plan. It may include some combination of surgery, radiation therapy, targeted monoclonal therapies, chemotherapy, or artificial immunotherapy. Surgical options may include transurethral resection, partial or complete removal of the bladder, or urinary diversion.[1] Then an artificial bladder can replace the body’s own bladder. This surgical technique can prolong lives to five years for those who have no faith in Holistic interventions and self-care. But what about after the five year mark ?
What if Holistic Oncology were able to help restore homeostasis and activate the immune system to the extent that would clear all of the dangersous circulating tumor and cancer stem cells and shrink the tumor to shreds ? Would it therefore not make sense to forego this obsession with biopsies and invasive testing that can spur and spread even more cancer cells and to immediately focus on what can reverse this disease ?
“Bladder cancer (BC) is ones of the most common cancer worldwide. It is classified in muscle invasive (MIBC) and muscle non-invasive (NMIBC) BC. NMIBCs frequently recur and progress to MIBCs with a reduced survival rate and frequent distant metastasis. BC detection require unpleasant and expensive cystoscopy and biopsy, which are often accompanied by several adverse effects. Thus, there is an urgent need to develop novel diagnostic methods for initial detection and surveillance in both MIBCs and NMIBCs. Multiple urine-based tests approved by FDA for BC detection and surveillance are commercially available. However, at present, sensitivity, specificity and diagnostic accuracy of these urine-based assays are still suboptimal and, in the attend to improve them, novel molecular markers as well as multiple-assays must to be translated in clinic”. (Source) (2)
In this perspective, there is growing evidence that “liquid biopsy” is effective insofar as the non invasive biomarkers for urologic malignancy is concerned. (Source)
Photodynamic diagnosis may improve bladder cancer surgical outcome (3), but this implies tissue invasiveness.
DNA- and RNA-based markers in body fluids such as blood and urine are promising potential markers in diagnostic, prognostic, predictive and monitoring urological malignancies. But they are not yet operational. Thus, circulating cell-free DNA, DNA methylation and mutations, circulating tumor cells, miRNA, IncRNA and mRNAs, cell-free proteins and peptides, and exosomes from urine specimens would be the best non invasive options.
However, in the conventional oncology system, proteomic and genomic data must to be validated in well-designed multicenter clinical studies before they can be employed in clinic oncology and this procedure can take many years and hundreds of millions of dollars.
“Current urinary biomarker research is a broad field that encompasses the evaluation of urinary proteins, DNA, RNA and EVs to detect signatures that can be used to predict the presence of bladder cancer and provide prognostic information. EVs in particular offer an exciting and novel perspective in the search for accurate bladder cancer biomarkers” (Source) (4)
Pending this research on exosomes, we do today have circulating tumor and stem cell biomarkers, what is called “liquid biopsy”, that comes from a simple blood draw and that has been shown to be reliable and way safer than tissue biopsies. (Source)
It is therefore the ACR Institute’s present position that using this test with clinical examination and common sense would be presently the least invasive and the most efficient and cost-friendly, thanks to which there would be a significant reduction in bladder cancer recurrence, once the HIP protocol and a holistic lifestyle are put in place.
Pr. Joubert (ACR Institute director)
To learn about the holistic and innovative techniques that can help to better control and reverse this health condition, consider scheduling a consult !
Text under construction
References
- “Bladder Cancer Treatment”. National Cancer Institute. 1 January 1980.
- Front Oncol. 2018; 8: 362.
- O’Brien T, Thomas K (November 2010). “Bladder cancer: Photodynamic diagnosis can improve surgical outcome”. Nature Reviews Urology. 7 (11): 598–9. doi:10.1038/nrurol.2010.183. .
- Curr Urol Rep. 2017; 18(12): 100.

Disclaimer: Nothing in this educational blog should be construed as medical advise
2019 (c). Advanced Cancer Research Institute and agents. All Rights Reserved